Did you know some breast and ovarian cancers are connected to pancreatic cancer? It could save your life.
Let’s begin by reminding you of Angelina Jolie and her recent decision to have both breasts removed to lower her risk for breast cancer because she has the BRCA1 gene – it stands for BReast CAncer. BRCA1 and 2 are genes that produce tumor suppressor proteins, proteins that help repair DNA mistakes that if left alone can lead to cancer. Some people inherit BRCA genes that don’t function properly and so they don’t make the tumor suppressor proteins. If you have one of those gene mutations, each of your children has a 50% chance of inheriting it from you.
A mutation in the BRCA 1 gene increases a woman’s risk of developing breast cancer by 55% to 65%; a mutation in the BRCA 2 gene increases a woman’s risk of developing breast cancer 45%. BRCA gene mutations cause about 5% to 10% of all breast cancer cases in the United States.
In the general population, about 1.4% of women will develop ovarian cancer. But among women who inherit the BRCA 1 mutation, there is a 39% risk of developing ovarian cancer. For those with a BRCA 2 mutation, the risk is 11% to 17% over her lifetime.
This is where the story gets personal. My wife Sharon has the BRCA 2 gene and she has done everything she can to lower her risk of cancer. She had her ovaries removed in her late forties to prevent ovarian cancer, a disease that killed many of the women in her family. And she has breast cancer screening every 6 months to find a cancer early if one appears.
But no one really talked with her about pancreatic cancer. Pancreatic cancer is a very deadly cancer that strikes about 1 in 76 people in the general population. However, if you carry the BRCA 2 mutation, you should also know that you have approximately a 3% to 5% of developing the disease. Dr. Goggins at Johns Hopkins has shown that as many as 10% of pancreas cancers are caused by inherited defects in the BRCA 2 gene. And that is exactly what happened to Sharon.
If you carry the BRCA 2 mutation, you have approximately a 3% to 5% risk of developing pancreatic cancer
It began with some very unusual symptoms – big, pale bowel movements that floated.
Tip number one – never ignore changes in your bowls.
Sharon had been having those changes for a month or so and felt a little tired, but other than that, she was not too far off her usual happy, healthy self. BMs aren’t a topic we usually discuss, so she didn’t mention it to me. Then she started losing weight – one pound a day. Since she wasn’t fat to begin with and wasn’t trying to lose weight that got us in to see her internist very quickly.
Tip number two – never ignore rapid weight loss.
Still not too worried. Sharon exercises and eats well and just had normal exams by her gynecologist and internist within the past six months with normal lab values. Tip number three – normal exams don’t always mean all is well.
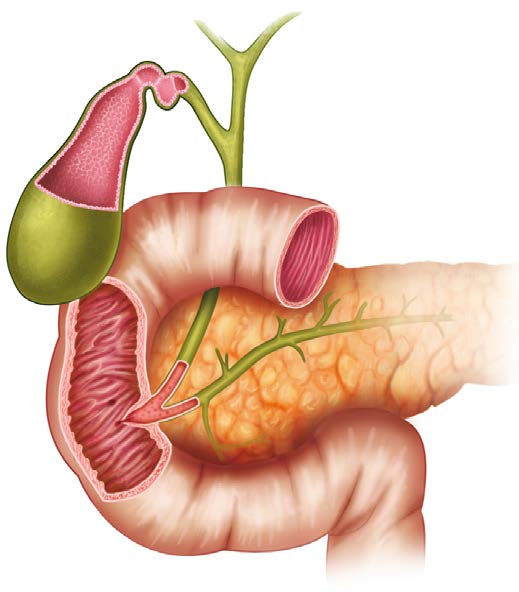
An ultrasound of her abdomen was done that day and it showed that the ducts from her pancreas to her duodenum (the start of her small intestines) and from her gall bladder to her duodenum were slightly dilated. That is when our adrenalin started pumping. The next day a CT exam showed a small half-inch “mass” in her pancreas. It was blocking the two ducts and that is why the ducts were slightly dilated. It’s also why the bowel movements were so different – the blocked ducts prevented digestive enzymes from getting into her intestines so the fat in her diet could not be broken down and digested, and fat makes stools float and look pale.
What happened afterwards is a story too long to entirely tell here, but here is the short version. Sharon had a biopsy done of the tumor in her pancreas. Sitting in the waiting room and waiting for these kinds of test results is nerve-racking. The nerve-racking got worse when the results came back as pancreatic cancer. A few days later Sharon had a belly button laparoscopy to look into her abdomen and see if the cancer had spread – it hadn’t. Then she enrolled in a proton beam radiation research study, which is more commonly used for brain tumors. This involved Sharon being in the “center of a triangle” and radiation coming from each of the three angles of the triangle into one “hot spot” that is focused on the tumor.
If you have the BRCA 2 mutation ask for a referral to an early detection pancreatic cancer screening center
Next came a large operation called a Whipple, followed by chemotherapy that was tailored to her BRCA 2 mutation. These last few sentences took months of time to complete. Over one year after the last chemotherapy, Sharon is disease free, and she is followed every three months for the next few years to make sure things stay that way.
The purpose of the story it to make you more aware of the connection between pancreatic cancer and the BRCA 2 gene mutation. You may be at increased risk if you have a strong family history of breast cancer or a member of your family had ovarian cancer. If that is your family history, talk with a genetic counselor about getting tested for the BRCA mutation.
If you know you have the BRCA 2 mutation ask your doctor to refer you to an early detection pancreatic cancer screening center so that you can get an individualized plan for screening and follow up. There are centers around the country that provide this type care. This approach is a new concept and it is important to allow high-risk individuals the best opportunity for early detection, which really is the best possible chance for a cure. For women and men who are BRCA 2 positive, it’s really important to know that your breasts and your pancreas are related.